The effect of a probiotic strain (Lactobacillus acidophilus) on the plaque formation of oral Streptococci
DOI:
https://doi.org/10.17305/bjbms.2011.2621Keywords:
adhesion, dental caries, Lactobacillus acidophilus, probiotic, StreptococciAbstract
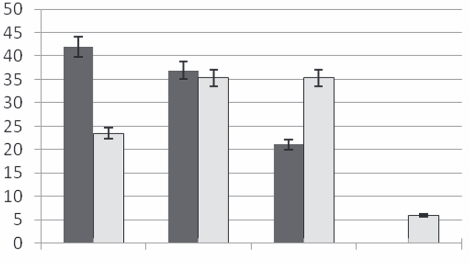
The objective of this study was to investigate the ability of biofilm formation among mutans and non mutans oral streptococci and to determine the effect of Lactobacillus acidophilus DSM 20079 as a probiotic strain on the adhesion of selected streptococcal strains on the surfaces. The sample comprised 40 isolates of oral streptococci from dental plaque and caries of volunteer persons. Streptococcus mutans ATCC35668 (no24) was as an standard strain. The probiotic strain was Lactobacillus acidophilus DSM 20079. The ability of biofilm formation was investigated with colorimetric method and the strongest isolates were selected. Then the effect of probiotic strain on the adhesion of streptococci isolates was determined in polystyrene microtiter plate simultaneously and 30 minutes before streptococci entrance to the system. The results showed that 42% of mutans streptococci were strongly adherent (SA) and in non mutans streptococci, only 23.5% of isolates were found strongly adherent. The strong biofilm forming bacterium isolated was Streptococcus mutans strain22. In the next step, in the presence of probiotic strain the streptococcal adhesion were reduced, and this reduction was non significantly stronger if the probiotic strain was inoculated to the system before the oral bacteria. The Lactobacillus acidophilus had more effect on adherence of mutans streptococci than non mutans streptococci with significant difference (p < 0.05). Adhesion reduction is likely due to bacterial interactions and colonization of adhesion sites with probiotic strain before the presence of streptococci. Adhesion reduction can be an effective way on decreasing cariogenic potential of oral streptococci.
Citations
Downloads
Downloads
Additional Files
Published
Issue
Section
Categories
License
Copyright (c) 2017 Bosnian Journal of Basic Medical Sciences

This work is licensed under a Creative Commons Attribution 4.0 International License.
How to Cite
Accepted 2017-11-01
Published 2011-02-20









