Analysis of Risk Factors, Localization and 30-day Prognosis of Intracerebral Hemorrhage
DOI:
https://doi.org/10.17305/bjbms.2008.2964Keywords:
intracerebral hemorrhage, risk factors, prognosisAbstract
Intracerebral hemorrhage is the deadliest, most disabling and least treatable form of stroke despite progression in medical science. The aim of the study was to analyze the frequency, risk factors, localization and 30-day prognosis in patients with intracerebral hemorrhage.
We analyzed 352 patients with intracerebral hemorrhage (ICH) hospitalized at the Department of Neurology Tuzla during a three-year follow up. The following data were collected for all patients in a computerized database: age, sex, risk factors (hypertension, heart diseases, diabetes and smoking) and CT findings. Stroke severity was estimated with Scandinavian Stroke Scale, ICH topography was specified by CT, and outcome at 1st month after onset included information on vital status and disability (modified Rankin Scale, mRS).
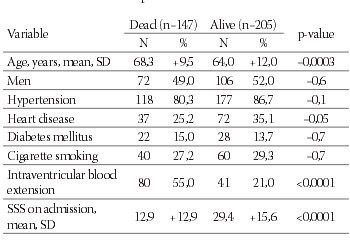
The most frequent risk factors were hypertension (84%), heart diseases (31%), cigarette smoking (28%) and diabetes mellitus (14%). The most frequent localization of ICH was multilobar (38%), internal capsule/basal ganglia region (36%) and lobar (17%). Within first month died 147 patients (42%). The highest mortality rate was in patients with brain stem (83%) and multilobar hemorrhage (64%). Factors independently associated with mortality were age (odds ratio 1,05 (95% confidence interval 1,02 to 1,08); p=0,001), stroke severity (OR 0,93 (0,92 to 0,95); p<0,0001), multilobar hemorrhage (OR 5,4 (3,0 to 9,6); p<0,0001) and intraventricular hemorrhage (OR 3,9 (2,2 to 7,1); p<0,0001). Favorable outcome at first month (mRS <2) had 45% of the surviving patients with ICH. The best outcome was for the patients with cerebellar hemorrhage (63%), while only 40% of the patients with hemorrhage in internal capsule/basal ganglia region had Rankin scale 2 or less.
Hypertension is the most frequent risk factor in patients with ICH. ICHs are mainly localized in lobar and internal capsule/basal ganglia regions. Independent predictors of mortality following ICH are age, hypertension, intraventricular blood extension and stroke severity. Mortality, as well as good outcome at 1 month, is related to the localization of bleeding.
Citations
Downloads
Downloads
Published
Issue
Section
Categories
How to Cite
Accepted 2018-01-13
Published 2008-05-20









