Rapid, multimodal, critical care knowledge-sharing platform for COVID-19 pandemics
DOI:
https://doi.org/10.17305/bjbms.2020.4934Keywords:
COVID 19, intensive care unit, critical illness, education, knowledge sharing, global healthAbstract
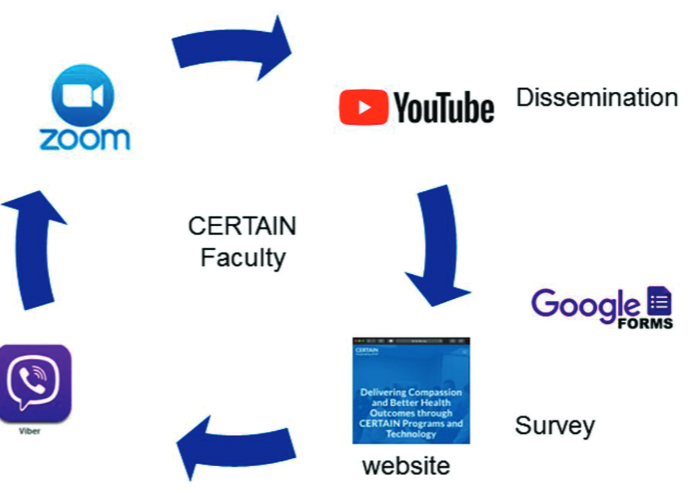
In many areas of the world, critical care providers caring for COVID-19 patients lacked specific knowledge and were exposed to the abundance of new and unfiltered information. With support from the World Health Organization, we created a multimodal tele-education intervention to rapidly share critical care knowledge related to COVID-19 targeting providers in a region of Southeastern Europe. We delivered 60-minute weekly interactive tele-education sessions over YouTubeTM between March 2020 and May 2020, supplemented by a dedicated webpage. The intervention was reinforced using a secure social media platform (ViberTM), providing continuous rapid knowledge exchange among faculty and learners. A high level of engagement was observed, with over 2000 clinicians participating and actively interacting over a 6-week period. Surveyed participants were highly satisfied with the intervention. Tele-education interventions using social media platforms are feasible, low-cost, and effective methods to share knowledge during the COVID-19 pandemic.
Citations
Downloads
Downloads
Additional Files
Published
Issue
Section
Categories
License
Copyright (c) 2020 Amra Sakusic, Dragana Markotic, Yue Dong, Emir Festic, Vladimir Krajinovic, Alan Sustic, Natasa Milivojevic, Milka Jandric, Srdjan Gavrilovic, Alexander Niven, Pedja Kovacevic, Ognjen Gajic

This work is licensed under a Creative Commons Attribution 4.0 International License.
How to Cite
Accepted 2020-10-24
Published 2021-02-01









