Nesfatin-1 and Vitamin D levels may be associated with systolic and diastolic blood pressure values and hearth rate in polycystic ovary syndrome
DOI:
https://doi.org/10.17305/bjbms.2015.432Keywords:
Nesfatin-1, vitamin D, polycystic ovary syndrome, insulin resistance, blood pressure, heart rateAbstract
Obesity, insulin resistance (IR), inflammation, and hyperandrogenism may lead to polycystic ovary syndrome (PCOS) and hypertension. Nesfatin-1 (N1) may be related to IR, obesity, and hypertension. Furthermore, a vitamin D (VD) deficiency is associated with hypertension and PCOS. We aimed to investigate N1 and VD levels in PCOS that have an effect on systolic and diastolic blood pressure (BP) and heart rate (HR).
This study included 54 patients with PCOS and 48 age-body mass index (BMI)-matched healthy controls. PCOS was diagnosed according to clinical practice guidelines. Ferriman-Gallwey scores (FGS) were calculated, while N1, VD, and other hormonal and biochemical parameters were measured for all subjects. Systolic and diastolic BP was measured as well. HR was calculated using an electrocardiogram.
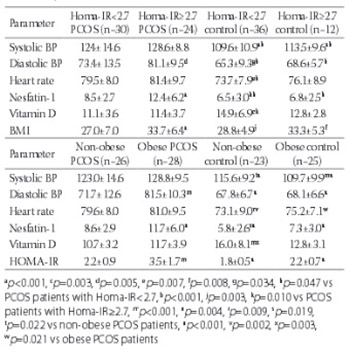
The levels of N1 (p < 0.001), high-sensitivity C-reactive protein (hs-CRP) (p = 0.036), homeostasis model assessment as an index of insulin resistance (HOMA-IR) (p < 0.001), systolic (p < 0.001) and diastolic (p < 0.001) BP and HR (p < 0.001) in the PCOS group were significantly higher than in the control group. However, the VD levels of the PCOS group were lower than the control group (p = 0.004). N1 had a strong positive correlation with BMI, HOMA-IR, hs-CRP, luteinizing hormone, systolic and diastolic BP, and HR. VD levels were negatively correlated with HOMA-IR and luteinizing hormone.
Elevated N1 and decreased VD levels may be related to the presence of high-normal BP or hypertension in PCOS subjects. N1 level may be associated with an increased BP due to its relation to inflammation and IR.
Citations
Downloads
References
Goodarzi MO, Dumesic DA, Chazenbalk G, Azziz R. Polycystic ovary syndrome: etiology, pathogenesis and diagnosis. Nat Rev Endocrinol 2011;7(4):219-231. http://dx.doi.org/10.1038/nrendo.2010.217.
Sahin FK, Sahin SB, Balik G, Ural UM, Tekin YB, Cure MC, et al. Does low pentraxin-3 levels associate with polycystic ovary syndrome and obesity? Int J Clin Exp Med 2014;7(10):3512-3519.
Wild RA, Carmina E, Diamanti-Kandarakis E, Dokras A, Escobar-Morreale HF, Futterweit W, et al. Assessment of cardiovascular risk and prevention of cardiovascular disease in women with the polycystic ovary syndrome: a consensus statement by the Androgen Excess and Polycystic Ovary Syndrome (AE-PCOS) Society. J Clin Endocrinol Metab 2010;95(5):2038-2049. http://dx.doi.org/10.1210/jc.2009-2724.
Diamanti-Kandarakis E, Dunaif A. Insulin resistance and the polycystic ovary syndrome revisited: an update on mechanisms and implications. Endocr Rev 2012;33(6):981-1030. http://dx.doi.org/10.1210/er.2011-1034. http://dx.doi.org/10.1210/er.2011-1034.
Oh-I S, Shimizu H, Satoh T, Okada S, Adachi S, Inoue K, et al. Identification of nesfatin-1 as a satiety molecule in the hypothalamus. Nature 2006;443(7112):709–712. http://dx.doi.org/10.1038/nature05162.
Stengel A, Mori M, Tache Y. The role of nesfatin-1 in the regulation of food intake and body weight: recent developments and future endeavors. Obes Rev 2013;14(11):859-870. http://dx.doi.org/10.1111/obr.12063.
Yosten GL, Redlinger L, Samson WK. Evidence for a role of endogenous nesfatin-1 in the control of water drinking. J Neuroendocrinol 2012;24(7):1078–1084. http://dx.doi.org/10.1111/j.1365-2826.2012.02304.x.
Könczöl K, Pinter O, Ferenczi S, Varga J, Kovacs K, Palkovits M, et al. Nesfatin-1 exerts long-term effect on food intake and body temperature. Int J Obes (Lond) 2005;36(12):1514–1521. http://dx.doi.org/10.1038/ijo.2012.2.
Yosten GL, Samson WK. The anorexogenic and hypertensive effects of nesfatin-1 are reversed by pretreatment with an oxytocin receptor antagonist. Am J Physiol Regul Integr Comp Physiol 2010;298(6):1642-1647. http://dx.doi.org/10.1152/ajpregu.00804.2009.
Su Y, Zhang J, Tang Y, Bi F, Liu JN. The novel function of nesfatin-1: antihyperglycemia. Biochem Biophys Res Commun 2010;391(1):1039-1042. http://dx.doi.org/10.1016/j.bbrc.2009.12.014.
Ademoglu EN, Gorar S, Carlıoglu A, Yazıcı H, Dellal FD, Berberoglu Z, et al. Plasma nesfatin-1 levels are increased in patients with polycystic ovary syndrome. J Endocrinol Invest 2014;37(8):715-719. http://dx.doi.org/10.1007/s40618-014-0089-2.
Garcia-Galiano D, Navarro VM, Roa J, Ruiz-Pino F, Sanchez-Garrido MA, Pineda R, et al. The anorexogenic neuropeptide, nesfatin-1, is indispensable for normal puberty onset in the female rat. J Neurosci 2010;30(23):7783–7792. http://dx.doi.org/10.1523/JNEUROSCI.5828-09.2010.
Kirbas A, Kirbas S, Anlar O, Turkyilmaz AK, Cure MC, Efe H. Investigation of the relationship between vitamin D and bone mineral density in newly diagnosed multiple sclerosis. Acta Neurol Belg 2013;113(1):43-47. http://dx.doi.org/10.1007/s13760-012-0123-0.
Cumhur Cure M, Cure E, Yuce S, Yazici T, Karakoyun I, Efe H. Mean platelet volume and vitamin D level. Ann Lab Med 2014;34(2):98-103. http://dx.doi.org/10.3343/alm.2014.34.2.98.
Luo C, Wong J, Brown M, Hooper M, Molyneaux L, Yue DK. Hypovitaminosis D in Chinese type 2 diabetes: lack of impact on clinical metabolic status and biomarkers of cellular inflammation. Diab Vasc Dis Res 2009;6(3):194-199. http://dx.doi.org/10.1177/1479164109337974.
Kozakowski J, Kapuscinska R, Zgliczynski W. Associations of vitamin D concentration with metabolic and hormonal indices in women with polycystic ovary syndrome presenting abdominal and gynoidal type of obesity. Ginekol Pol 2014;85(10):765-770.
ESHRE/ASRM. Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group. Revised 2003 consensus on diagnostic criteria and longterm health risks related to polycystic ovary syndrome. Fertil and Steril 2004;8:19-25.
Rahman M, Berenson AB. Accuracy of current body mass index obesity classification for white, black, and Hispanic reproductive-age women. Obstet Gynecol 2010;115(5):982-988. http://dx.doi.org/10.1097/AOG.0b013e3181da9423.
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985;28(7):412-419. http://dx.doi.org/10.1007/BF00280883.
Guleria AK, Syal SK, Kapoor A, Kumar S, Tiwari P, Dabadghao P. Cardiovascular disease risk in young Indian women with polycystic ovary syndrome. Gynecol Endocrinol 2014;30(1):26-29. http://dx.doi.org/10.3109/09513590.2013.831835.
Bajuk Studen K, Jensterle Sever M, Pfeifer M. Cardiovascular risk and subclinical cardiovascular disease in polycystic ovary syndrome. Front Horm Res 2013;40:64-82. http://dx.doi.org/10.1159/000341838. http://dx.doi.org/10.1159/000341838.
Hadi HA, Carr CS, Al Suwaidi J. Endothelial dysfunction: cardiovascular risk factors, therapy, and outcome. Vasc Health Risk Manag 2005;1(3):183-198.
Vaneckova I, Maletinska L, Behuliak M, Nagelova V, Zicha J, Kunes J. Obesity-related hypertension: possible pathophysiological mechanisms. J Endocrinol 2014;223(3):63-78. http://dx.doi.org/10.1530/JOE-14-0368.
Zachurzok-Buczynska A, Szydlowski L, Gawlik A, Wilk K, Malecka-Tendera E. Blood pressure regulation and resting heart rate abnormalities in adolescent girls with polycystic ovary syndrome. Fertil Steril 2011;96(6):1519-1525. http://dx.doi.org/10.1016/j.fertnstert.2011.09.043.
Sahin SB, Cure MC, Ugurlu Y, Ergul E, Gur EU, Alyildiz N, et al. Epicardial adipose tissue thickness and NGAL levels in women with polycystic ovary syndrome. J Ovarian Res 2014;7:24. http://dx.doi.org/10.1186/1757-2215-7-24.
Tsuchiya T, Shimizu H, Yamada M, Osaki A, Oh-I S, Ariyama Y, et al. Fasting concentrations of nesfatin-1 are negatively correlated with body mass index in non-obese males. Clin Endocrinol (Oxf) 2010;73(4):484-490. http://dx.doi.org/10.1111/j.1365-2265.2010.03835.x.
Shimizu H, Ohsaki A, Oh-I S, Okada S, Mori M. A new anorexigenic protein, nesfatin-1. Peptides 2009;30(5):995-998. http://dx.doi.org/10.1016/j.peptides.2009.01.002.
Feijoo-Bandin S, Rodriguez-Penas D, Garcia-Rua V, Mosquera-Leal A, Otero MF, Pereira E, et al. Nesfatin-1 in human and murine cardiomyocytes: synthesis, secretion, and mobilization of GLUT-4. Endocrinology 2013;154(12):4757-4767. http://dx.doi.org/10.1210/en.2013-1497.
Aksu O, Aydın B, Doguç DK, Ilhan I, Ozturk O, Altuntas A, et al. The evaluation of Nesfatin-1 levels in patients with OSAS associated with metabolic syndrome. J Endocrinol Invest 2015;38(4):463-469. http://dx.doi.org/10.1007/s40618-014-0216-0.
Downloads
Additional Files
Published
Issue
Section
Categories
How to Cite
Accepted 2015-05-12
Published 2015-07-09









