The Possible Role of Early Post-Transplant Inflammation in Later Anemia in Kidney Transplant Recipients
DOI:
https://doi.org/10.17305/bjbms.2009.2786Keywords:
leukocytosis, graft rejection, erythropoietin, kidney transplantation, inflammationAbstract
Delayed kidney graft function and acute rejection in the early post-transplant period affect both short and long-term allograft survival. Allograft rejection, as an inflammatory state, results in increased eryth-ropoietin resistance, which leads to decreased haemoglobin (Hb) level. We conducted this study to evaluate whether inflammation in the early post-transplant period could predict later anemia.
This is a retrospective cohort study based on the analysis of 64 existing clinical records. Predictor. White blood cells (WBC) count obtained by the end of the first week post-transplant (W1). Covariates. Donor’s age, recipient’s age and sex. Outcome. Anemia identified at 12 months (M12) post engraftment.
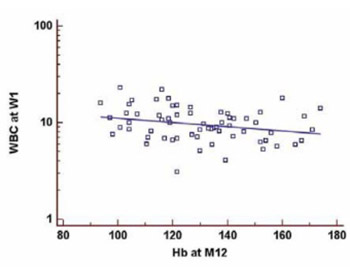
Median WBC count at W1 was 9,5 x103^L (5th - 95th percentile 5,2 x103^L -17,8 x 103/μΚ). Mean Hb values at M12 were 129,9 ± 20,3 g/L, in males 136,2 ± 20,1 g/L and in females 119,4 ± 16,2 g/L. The significant correlation was found between WBC at W1 and Hb at M12. Pearson coefficient of correlation r was -0,26, and 95% confidence interval (CI) for r was -0,47 to -0,015 (p=0,03). Univariate logistic regression showed significant association between WBC at W1 and Hb at M12 (OR 1,20; 95% CI 1,04 to 1,39, p=0,01). After the adjustment for donor’s and recipient’s age by transplantation and recipient’s sex, multiple regression showed that WBC count remained predictive of anemia at M12 (OR 1,17; 95% CI 1,01 to 1,36, p=0,03).
Early post-transplant inflammatory response predicts later anemia in kidney transplant recipients. An increase in WBC count in the first week post-transplant by 109/L increases the risk for anemia after twelve months by 17%.
Citations
Downloads
Downloads
Published
Issue
Section
Categories
How to Cite
Accepted 2017-12-07
Published 2009-11-20









